If you have bile duct cancer that has come back after surgery (is ‘recurrent’), that means some cancer cells were left behind and have started to grow. You will need another type of treatment to try and control the cancer.
If you have advanced bile duct cancer, the aim of treatment is to try and shrink the cancer and relieve any symptoms you might be having.
In either case, you may have:
- treatment to relieve a blockage in your bile ducts
- chemotherapy
- radiotherapy
- a targeted (biological) therapy
- treatments to relieve symptoms
Treatment to relieve a blocked bile duct
If you have a blocked bile duct, you are likely to develop jaundice [LINK symptoms page]. As well as causing yellowing of the skin and eyes, this can make you feel very unwell if it isn’t treated.
The usual way to help with this is to put in a stent. This is a tube about as thick as a ball-point pen refill and 5 to 10cm long (2 to 4 inches). It holds a bile duct open so that bile can flow into the small bowel.
You may have a stent put in via a tube down your throat and into the small bowel (an endoscopy) – an ERCP [LINK Tests#ERCP]. Or you may have it put in through a small cut in your skin – a PTC procedure [LINK Tests#PTC].
A stent will relieve jaundice symptoms, so your general health will improve and you will be able to digest food again normally. Stents usually need to be replaced every 3 to 4 months as they can become blocked, and cause an infection (cholangitis). If you have:
- high temperature/fever
- jaundice
- chills, shivering
contact your doctor or CNS (Clinical Nurse Specialist). Untreated, cholangitis can be serious. You may need antibiotics and a replacement stent.
Chemotherapy
This is using anti-cancer (‘cytotoxic’) drugs to destroy cancer cells. The advantage of chemotherapy is that it circulates throughout the body so can also kill cancer cells that have spread. You may have chemotherapy to try and shrink a cancer that can’t be removed with surgery, which should help with any symptoms you have.
Chemotherapy treatments for advanced bile duct cancer is usually a combination of two chemo drugs called gemcitabine (Gemzar®) and cisplatin. There is more about this type of chemo [LINK inoperable BDC page #chemo] in the page on bile duct cancer that can’t be removed [LINK inoperable BDC page].
If you’ve already had treatment with gemcitabine and cisplatin and your cancer has started to grow again, your doctor may suggest a different chemo combination. The most likely is called mFOLFOX. This includes the chemo drugs 5-FU and oxaliplatin with another drug called folinic acid, which helps the chemotherapy to work.
You have mFOLFOX through a drip (intravenous infusion). You have the 5FU through a pump that stays in place for 24 hours (you can go home with it attached). You have treatment in the hospital out patients department, over 2 days, followed by 12 days with no treatment. This 2-week period is called a cycle of treatment. How many cycles you have will depend on how much it is helping you.
Common side effects of chemotherapy include:
- increased risk of infection
- feeling or being sick
- feeling very tired (fatigue)
Some side effects are specific to particular chemo drugs. With mFOLFOX, you may have:
- diarrhoea
- numbness and tingling in your fingers and toes
- a sore mouth and mouth ulcers
Sometimes people have an allergic reaction when they are having oxaliplatin. Tell your nurse if you feel breathless, or have chest pain, a rash or itching eyes.
Radiotherapy
This type of treatment uses high energy X-rays directed at the cancer. Like chemo, radiotherapy kills dividing cells, so cancer cells are more sensitive to it than normal cells. It’s used less often for bile duct cancer. But your doctor may suggest it if you have symptoms and they think it could shrink the cancer and help relieve them.
Having the treatment is a bit like having an X-ray. You can’t feel it and each treatment takes a few minutes. You may have just one treatment, or several treatments over a few days. Beforehand, you’ll have a longer appointment for radiotherapy planning. This involves having a scan, which the radiotherapist will use to work out exactly where to direct the treatment.
Radiotherapy can have side effects, but these are less likely if you’re only having a short course of treatment.
There is more about radiotherapy [LINK main Rtx page] in the liver cancer treatment [LINK main treatment menu] section.
Targeted therapy
Targeted cancer drugs are the newest type of cancer treatment. They are sometimes called biological therapies. Some intrahepatic bile duct cancers have particular gene changes that can be targeted by these drugs.
Your doctor may suggest a drug called pemigatinib. This works by blocking the chemical signals that tell cancer cells to divide and grow. These ‘growth factors’ are often the same as those used by normal cells, but produced in abnormally large amounts. That’s why the treatments can have side effects – while you are taking it, the treatment blocks signals from normal cells too.
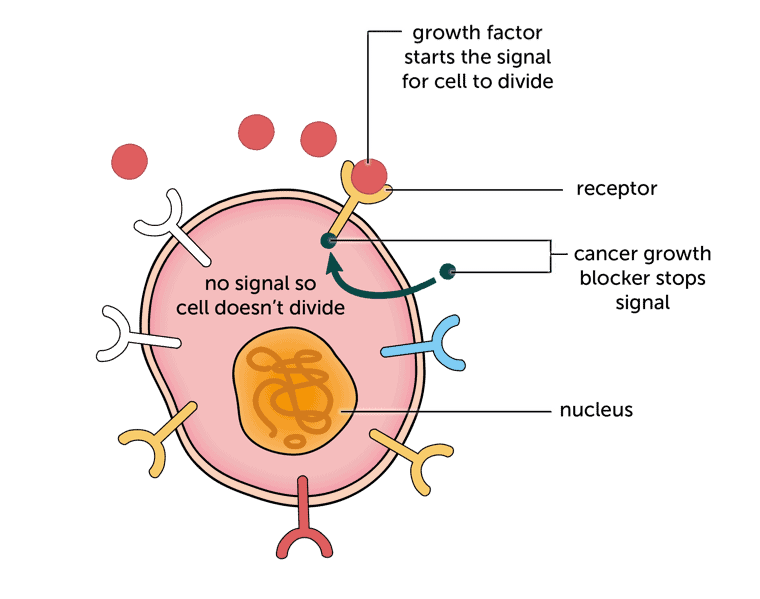
Pemigatinib will only help if your cancer cells produce the growth factor it blocks (or ‘targets’). This is called FGFR2, which stands for Fibroblast Growth Factor Receptor 2. Your doctor may call this a ‘marker’.
Your doctor will test a sample of your cancer before you start treatment. People with the same cancer type can have different markers. So you may come across other people with bile duct cancer who are having different treatments to you.
You have pemigatinib as a tablet that you take at the same time each day for 2 weeks. Then you have a week off. You can continue to take it for as long as it’s helping.
Pemigatinib can have side effects, including:
- changes in normal levels of sodium and phosphate in the blood (your doctor will test for this regularly)
- digestive upsets, including feeling sick, diarrhoea or constipation
- changes in taste and sore mouth
- dry skin and nail changes
- hair loss
- aching muscles
- tiredness
There is more about targeted therapies [LINK main Targeted tx page] in the liver cancer treatment [LINK main treatment menu] section.
Immunotherapy
There is some research evidence that an immunotherapy drug may help to treat advanced bile duct cancer alongside chemotherapy. In trials, patients did better with this than with chemotherapy alone.
This treatment, called durvalumab is a type of immunotherapy. It blocks a protein that cancer cells make. This protein stops your immune system finding the cancer cells. You have it with two chemotherapy drugs usually used to treat bile duct cancer – gemcitabine and cisplatin.
Treatments to relieve symptoms
If you are having pain or feeling sick, your doctor will be able to give you painkillers or anti-sickness medicines. These days, these often work very well. Do tell your doctor or nurse if they aren’t helping you. There are a lot of different types of both, so another anti-sickness or pain medication may work better for you. Our section on treating symptoms of advanced liver cancer has more information that you may find helpful. This includes suggestions of ways to cope with tiredness and problems with diet.
