There are a number of tests you may have if your doctor suspects you have a liver, gallbladder or bile duct cancer. You can also look at the sections on these types of cancer for information on the diagnostic tests used for each.
There is also information below on what happens after your tests
Ultrasound
This is a type of scan that uses soundwaves to build up a picture of the liver, bile ducts and surrounding organs. It is a common test for several types of liver cancer.
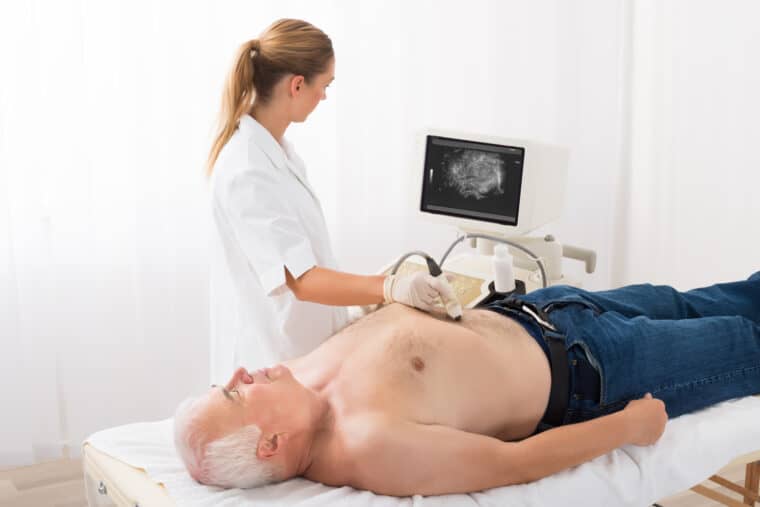
Ultrasound scans are completely painless and usually take less than half an hour.
To have the scan, you lie on your back and have a small amount of gel spread over your abdomen. The gel helps the ultrasound probe to produce clearer pictures. The radiographer moves the probe back and forth over your abdomen, while checking the pictures on a monitor. You may be able to see the pictures during your scan. The scan report will be sent to your consultant.
CT scan
CT stands for computerised tomography. The scanner takes a series of X-rays in cross-section and a computer puts them together to give a detailed picture of your body organs. The scan is completely painless and takes about half an hour.
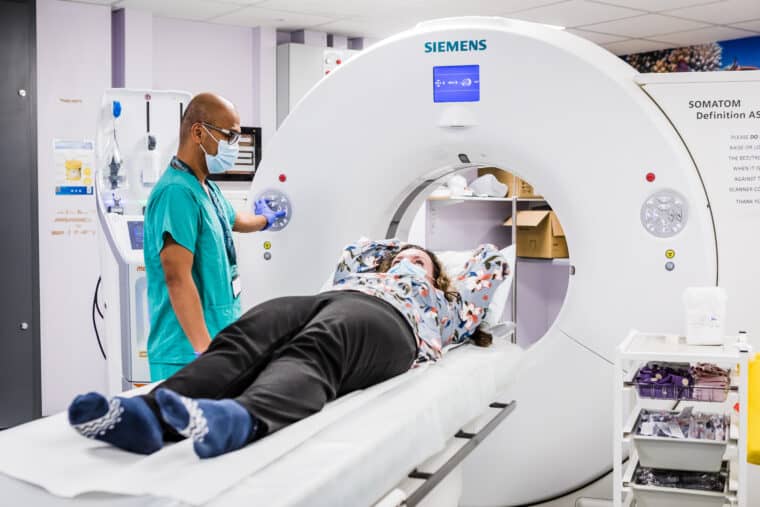
Because it’s an X-ray, a CT scan does expose you to some radiation. But it’s a relatively small amount and the benefit in diagnosing you outweighs any risk. There is background radiation from the environment that we’re all exposed to every day. A CT of your tummy (abdomen) exposes you to about the same as 4.5 years of background radiation.
Your doctor may ask you not to eat or drink for a few hours before your scan. Let them know if that’s a problem, for example if you have diabetes.
You usually have to change into a hospital gown when you get to the hospital. You may have a drink or injection of medical dye just before your scan. This is called ‘contrast’ and helps make the scan clearer. The scanner looks like a ring doughnut on end. You lie on the scanner bed and this moves in and out of the doughnut while you have your scan. The scan report will be sent to your consultant.
MRI scan
MRI stands for magnetic resonance imaging. It uses magnets and radio waves to produce images of the inside of the body. MRI scans show soft tissues more clearly than CT scans.
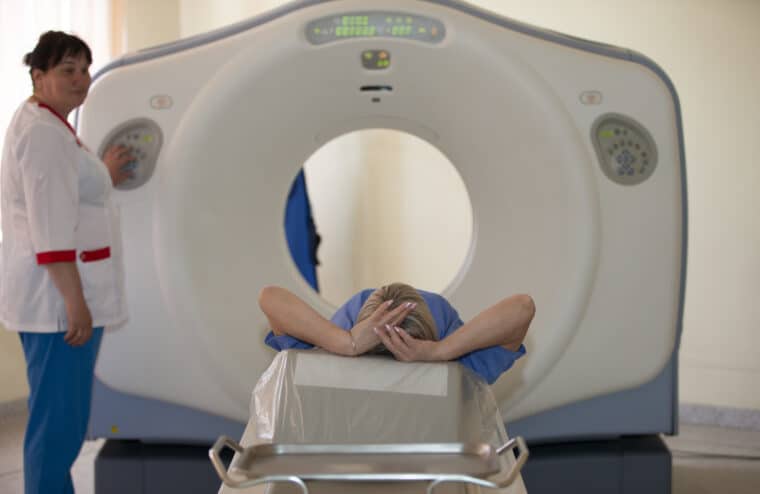
MRIs are painless and take about half an hour. As they use magnets, there is no radiation risk. MRI scanners can be very noisy, so you’ll have headphones to wear and can bring your own music to listen to during the scan if you like. Because the scanner bed moves into the scanner tube, some people feel shut in (claustrophobic). Tell your radiographer if you think that will be a problem for you.
Because of the magnets, you have to remove all jewellery and any clothing containing metal (bra straps, belt buckles, for instance) before your scan. You’ll also have to remove dentures and hearing aids that have any metal parts.
Some medical implants are fine as they are made of titanium so aren’t affected by magnets. But your radiographer will need to know in advance if you have any implants, such as a pacemaker, replacement heart valves or cochlear implants. The radiographer will go through some medical questions with you before your scan to make doubly sure it’s completely safe for you to go ahead. Do contact your doctor before your scan if you have any concerns.
You may have an injection of a dye called contrast medium, which makes the scan images clearer. This may make you feel warm, sick or dizzy but this is usually mild and doesn’t last long.
You usually change into a hospital gown when you get to the hospital. You then lie on the scan bed, which slides into a long tube. It’s important to keep still when the images are being taken. To help with this, your radiographer will ask you to hold your breath for a few seconds at times during your scan. You may feel hot and have tingling in your hands and feet. This is completely normal. You’ll be able to hear and speak to the person operating the scanner throughout, so you can say if you want to stop at any point. The scan report will be sent to your consultant.
Endoscopic Ultrasound
This is an ultrasound scan done from inside the body. The doctor uses an endoscope, which is a long, bendy tube that you swallow. it has a very small ultrasound probe attached to the end. The doctor passes the tube down your throat, through your stomach and into the small bowel. Then they can see the liver, gallbladder and bile ducts through the bowel wall . They can also take tissue samples (biopsies) during the test.
This test usually takes about half an hour. You may need to change into a hospital gown. You can have a sedative beforehand if you are anxious. Before putting the tube in, the doctor will spray anaesthetic on the back of your throat. This numbs it and makes it easier for you to swallow the tube.
If you’ve had a sedative, your radiographer may ask you to stay for a while after the test. You won’t be able to drive after sedation, or go home alone. So you’ll need a friend or relative to come with you. You shouldn’t eat or drink for an hour until the anaesthetic spray wears off, as it can affect your ability to swallow safely.
PET scans
PET stands for Positron Emission Tomography. It shows up cells that are very active, as cancer cells are. It can help to show whether any abnormal looking areas on other scans are cancerous or scar tissue from something else.
You have an injection of a ‘radiotracer’ (a very small amount of a radioactive substance) into a vein. This is often a form of sugar, which active cells use more of than inactive ones. The sugar collects in the active cells and because it’s radioactive, it highlights them on the scan.
The scan takes between 30 minutes and an hour. You have to be there an hour before it starts to have your injection. You need to be on time as the injection decays and the scan may be cancelled if you’re late.
Your doctor may ask you not to eat or drink anything except water for around 6 hours before the scan. They may also ask you not to exercise for 24 hours beforehand.
Because PET scans measure the uptake of sugar, people with diabetes will have special instructions about their medication and when they should eat before the scan. A PET scan may not be possible if your diabetes isn’t well controlled.
You usually change into a gown when you get to the hospital. You lie on a bed to have the injection. After that, you have to keep still and quiet as moving and talking will affect where the tracer collects.
After an hour, you have your scan, which takes up to an hour. Again, it’s important to try and keep still and not talk. If you think you’ll have trouble lying still for an hour, speak to your radiographer.
After the scan, you need to drink plenty of water to flush the tracer out of your system. The radiation will be out of your body within a few hours. As it’s such a small dose, the radiation is no risk to you, but your radiographer may ask you not to get too close to babies or pregnant women for a few hours after your scan.
PTC
This stands for ‘percutaneous transhepatic cholangiography’. PTC shows up any blockages or abnormalities inside the bile duct.
Percutaneous (say: per-kew-tane-ee-us) means through the skin. You have a local anaesthetic injection to numb the area over your liver. Then the doctor puts a very fine needle through the skin and into the liver. They inject dye into a bile duct inside the liver, so that it shows up more clearly on an X-ray. If needed, they can also take a tissue sample (biopsy) from the liver or put in a stent to help drain bile.
You have antibiotics before and after PTC to help prevent infection. You will have to stay in hospital for at least one night.
Biopsy
A biopsy is a small sample of tissue. The doctor sends the sample to a medical laboratory, where it is examined for signs of disease, including cancer.
Your doctor may use an ultrasound or CT scan to ‘guide’ the biopsy and make sure they take tissue samples from areas that look abnormal on the scan.
There are a number of ways of taking a biopsy. You may have one taken using a needle, through the skin above the liver. The doctor will numb the area with local anaesthetic first. This is called a percutaneous (say: per-cue-tane-ee-us) biopsy. Or you may have biopsies taken during a laparoscopy (see below) or during surgery.
If it’s possible to reach the right area, your doctor may be able to take tissue samples during any test that uses an endoscope. You may have this type of biopsy if you’re having tests for bile duct cancer.
The liver has a very rich blood supply. So there is a risk of bleeding after a sample has been taken from the liver. To reduce the risk of bleeding, your doctor will ask you to stay in bed for 6 hours afterwards. So you may need to spend the night in hospital.
It often takes a couple of weeks or more to get biopsy results if the sample has to be ‘stained’.
That means it’s treated with a dye that helps the cells to show up more clearly and makes diagnosis easier.
Laparoscopy
A laparoscopy is really a small operation. The doctor makes a small cut (incision) and uses a tube with a camera attached (the laparoscope) to examine the area. As with an endoscopy, they can use small instruments through the tube to take tissue samples if they see anything that looks abnormal.
You have a general anaesthetic so will be asleep during the procedure. You can’t eat or drink for 6 hours beforehand, because of the anaesthetic. Afterwards you’ll have stitches and a dressing on the wound. You may be able to go home the same day, but may need to stay in hospital overnight.
Blood tests
If you’re having tests for liver cancer, your GP or specialist will do some blood tests. These are usually a standard set that used to be called ‘liver function tests’ but are now just called liver blood tests. They check the levels of a number of different substances made by the liver to see if any are abnormal.
Depending on the type of liver cancer, you are having investigated, you may have a blood test for a ‘cancer marker’. A marker is a substance that can be measured in a blood tests and is made by cancer cells.
Hepatocellular liver cancer (HCC) cells sometimes make a substance called AFP. This stands for alpha-fetoprotein. It’s made by livers of newborn babies and levels are normally very low in adults. If your HCC makes AFP, the blood test can help to tell your doctor how your treatment is going and whether the cancer has come back after treatment. Similarly in bile duct cancer (cholangiocarcinoma), levels of a substance called CA19.9 may be raised.
Cancers vary, even within the same type. So your HCC or bile duct cancer may not produce markers.
Molecular Profiling
This is a test on your biopsy, rather than on you! It means taking a sample of your cancer and testing it to see which particular gene changes the cancer cells carry. Cancer cells have changes in their DNA that help them survive and grow uncontrollably. The most recent developments in cancer treatment target these changes – so are called targeted or biological drugs. To know which of these are likely to work for you, your doctor has to know whether your cancer cells have the target that each drug attacks.
There is more about what targeted treatment is in our general info on liver cancer treatment.
After your tests
Waiting for test results can be nerve wracking. It could take a week or two and that may seem like forever. There’s no right or wrong way to deal with this situation. Many people try to carry on as normal – others find their concentration is too poor. Try not to bottle up how you are feeling. If you don’t feel you can talk to relatives or friends, a counsellor may help.
In the meantime, be reassured that you haven’t been forgotten – work on your case is going on. Scan reports have to be made and sent to your specialist for review. If you’ve had biopsies taken, the sample may need to be ‘stained’ and that takes a few days.
A team of specialists will need to look at your results to decide the best course of action. This is called a ‘multi-disciplinary team’ or MDT for short. It will include a surgeon, medical cancer specialist, specialist nurse, pathologist (specialist in studying cells and biopsies) and a radiologist (an expert in reading scans and X-rays). Once they’ve met and discussed how best to treat you, you will have an appointment to go through your diagnosis and any planned treatment.
When you go to get your results, it’s a good idea to take someone with you. This isn’t only for moral support. It’s so that there are two of you to remember what’s been said. Your relative or friend could take notes for you and remind you of any questions you particularly wanted to ask.
Content last reviewed: October 2022
Next review date: October 2025
